Cervical cancer screening is evolving, and a significant change has been implemented: the recommended screening age has been lowered to 25. This adjustment reflects advancements in medical understanding and aims to improve early detection of cervical cancer. This change has the potential to significantly impact women’s health and the way healthcare providers approach cervical cancer prevention.
This shift to age 25 for screening is based on the latest medical research and is intended to identify precancerous changes or early-stage cancer sooner, leading to more effective treatment and better outcomes. This article will explore the rationale behind this change, the screening methods involved, the importance of patient education, potential challenges, and a comparison with international guidelines.
Impact of Lowering the Cervical Cancer Screening Age to 25

Source: enhancv.com
The decision to lower the cervical cancer screening age to 25 represents a significant shift in preventative healthcare strategies. This change is designed to enhance early detection and improve patient outcomes. It reflects a deeper understanding of cervical cancer development and the potential benefits of earlier intervention.
Rationale for Lowering the Screening Age
The primary rationale behind lowering the screening age is rooted in the evolving understanding of cervical cancer and its precursors. This understanding is informed by ongoing research and improved diagnostic tools.The age of 25 was selected because:
- Cervical cancer is often caused by the human papillomavirus (HPV). HPV infection is very common in young adults, and most infections clear up on their own. However, some infections can persist and lead to cervical cancer.
- Screening at age 25 allows for detection of persistent HPV infections and early precancerous changes.
- The incidence of cervical cancer is increasing in women in their late 20s and early 30s.
- Advances in screening methods, such as HPV testing, have improved the accuracy and effectiveness of early detection.
Potential Benefits of Earlier Screening
Earlier screening offers several potential benefits, primarily centered on increased detection rates and improved patient outcomes.Potential benefits include:
- Increased Detection Rates: Screening at a younger age increases the likelihood of detecting precancerous changes and early-stage cancers.
- Improved Patient Outcomes: Early detection allows for timely intervention, such as treatment of precancerous lesions, which can prevent the development of invasive cancer. This leads to a higher chance of successful treatment and improved survival rates.
- Reduced Mortality: By detecting and treating cervical cancer at an earlier stage, screening can significantly reduce mortality rates.
- Reduced Morbidity: Early intervention often involves less aggressive treatment, leading to fewer side effects and a better quality of life for patients.
- Cost-Effectiveness: While there are initial costs associated with increased screening, early detection and treatment can be more cost-effective in the long run than treating advanced-stage cancers.
Comparison of Cervical Cancer Incidence and Mortality Rates (Hypothetical Data)
Analyzing hypothetical data provides insight into the potential impact of the age change.Here’s a comparison of cervical cancer incidence and mortality rates in the 25-29 age group before and after the change (Hypothetical Data):
| Demographic | Incidence Rate (per 100,000) Before Age Change | Incidence Rate (per 100,000) After Age Change | Mortality Rate (per 100,000) Before Age Change | Mortality Rate (per 100,000) After Age Change |
|---|---|---|---|---|
| Overall | 8.2 | 6.5 | 1.9 | 1.2 |
| White Women | 7.0 | 5.8 | 1.6 | 0.9 |
| Black Women | 11.5 | 9.2 | 2.8 | 1.8 |
| Hispanic Women | 9.8 | 7.9 | 2.3 | 1.5 |
Note: The data presented above are hypothetical and for illustrative purposes only. Actual rates may vary.
Projected Impact of the Age Change Over 5 Years
The following table provides a projected impact of the age change on the number of women screened, the number of cancers detected, and the potential reduction in deaths over a 5-year period.
| Metric | Year 1 | Year 2 | Year 3 | Year 4 | Year 5 |
|---|---|---|---|---|---|
| Number of Women Screened (increase) | +100,000 | +110,000 | +120,000 | +130,000 | +140,000 |
| Number of Cancers Detected (increase) | +50 | +60 | +70 | +80 | +90 |
| Potential Reduction in Deaths | -5 | -7 | -9 | -11 | -13 |
| Number of Precancerous Lesions Detected (increase) | +300 | +330 | +360 | +390 | +420 |
Note: These projections are based on hypothetical data and are subject to change based on various factors.
Methods and Procedures for Cervical Cancer Screening at Age 25
Lowering the screening age to 25 necessitates a clear understanding of the methods, protocols, and processes involved in cervical cancer screening. This ensures effective early detection and appropriate management of any abnormalities. This section details the standard screening practices, provider guidelines, and the typical screening process, providing a comprehensive overview for both patients and healthcare professionals.
Standard Screening Methods
Cervical cancer screening primarily relies on two methods: the Pap test and HPV testing. These tests can be used individually or in combination to detect precancerous changes or the presence of the human papillomavirus (HPV), a primary cause of cervical cancer.The Pap test, also known as a Papanicolaou test, involves collecting cells from the cervix. A healthcare provider uses a small brush or spatula to gently scrape cells from the cervix.
These cells are then sent to a laboratory for examination under a microscope to check for any abnormal changes.HPV testing, on the other hand, detects the presence of HPV in the cervical cells. The same sample collected for a Pap test can often be used for HPV testing. Some providers may perform HPV testing separately, using a different collection method.
The test looks for the presence of high-risk HPV types, which are the ones most likely to cause cervical cancer.
Guidelines and Protocols for Healthcare Providers
Healthcare providers follow specific guidelines and protocols when screening women aged 25. These guidelines ensure consistent and effective screening practices.The primary guideline recommends that women aged 25 should begin cervical cancer screening with either a primary HPV test or a co-test (Pap test and HPV test together). If the primary HPV test is negative, the next screening can be done in five years.
If the Pap test and HPV test are done together (co-testing), and both are negative, the next screening can be done in five years. If only a Pap test is done, then the next screening is done in three years.Providers should also be aware of a patient’s medical history, including previous screening results, HPV status, and any risk factors, such as a family history of cervical cancer or a history of smoking.
This information helps tailor the screening approach and determine the frequency of screenings.
Typical Screening Process: A Step-by-Step Guide
The screening process involves several steps, from patient education to follow-up care.The screening process begins with patient education. The healthcare provider explains the importance of cervical cancer screening, the screening methods used, and the potential benefits and risks. The provider also answers any questions the patient may have.The provider then collects the sample. This involves using a speculum to visualize the cervix and collecting cells using a brush or spatula.
The sample is then sent to a laboratory for analysis.The laboratory analyzes the sample and provides the results to the healthcare provider. The provider then contacts the patient to discuss the results.If the results are normal, the patient is advised on the appropriate screening interval based on the guidelines. If the results are abnormal, the patient is informed about the findings and the next steps.Follow-up care may include repeat testing, colposcopy, or other procedures, depending on the results.
Abnormal Results and Follow-up Procedures
Abnormal screening results require specific follow-up procedures.
- Negative for Intraepithelial Lesion or Malignancy (NILM): No abnormalities detected. Routine screening intervals are followed.
- Atypical Squamous Cells of Undetermined Significance (ASC-US): Mild cellular changes.
- Follow-up: Repeat Pap test or HPV testing in one year.
- Low-Grade Squamous Intraepithelial Lesion (LSIL): Mild precancerous changes.
- Follow-up: Colposcopy.
- High-Grade Squamous Intraepithelial Lesion (HSIL): More severe precancerous changes.
- Follow-up: Colposcopy with possible biopsy and treatment, such as loop electrosurgical excision procedure (LEEP).
- Atypical Glandular Cells (AGC): Abnormal cells from the glandular tissue.
- Follow-up: Colposcopy, endocervical sampling, and potentially endometrial sampling.
- Squamous Cell Carcinoma or Adenocarcinoma: Cancerous cells present.
- Follow-up: Immediate referral to a gynecologic oncologist for further evaluation and treatment.
Patient Education and Awareness Regarding Cervical Cancer Screening

Source: medium.com
Educating women about cervical cancer screening is crucial for promoting early detection and improving outcomes. Comprehensive patient education empowers women to make informed decisions about their health, understand the screening process, and address any anxieties they may have. This section focuses on the importance of patient education, provides examples of educational materials, addresses common misconceptions, and Artikels the patient journey.
Importance of Patient Education
Patient education plays a vital role in increasing screening rates and reducing cervical cancer mortality. When women are well-informed, they are more likely to undergo regular screenings and seek prompt medical attention if necessary. Education helps dispel myths, reduce fear, and foster a sense of control over their health.
Examples of Educational Materials
Several educational materials can be used to inform women aged 25 about cervical cancer screening. These materials should be clear, concise, and culturally sensitive.
- Brochures and Fact Sheets: These materials provide concise information about cervical cancer, its causes, the screening process (Pap test and HPV test), and the benefits of early detection. They can be distributed in clinics, doctors’ offices, and community centers. The brochure should explain, in simple terms, what happens during a Pap smear and an HPV test, including how long the procedure takes and what to expect afterward.
- Websites and Online Resources: Websites maintained by reputable organizations, such as the American Cancer Society and the National Cancer Institute, offer comprehensive information about cervical cancer, screening guidelines, and risk factors. These resources should be easily accessible and mobile-friendly. Websites should feature interactive quizzes to test a patient’s understanding of the information and include videos demonstrating the screening process.
- Videos: Short videos can visually explain the screening process, making it easier for women to understand what to expect. These videos should feature diverse representation and be available in multiple languages. The video should show a healthcare provider explaining the procedure step-by-step, including the use of a speculum and the collection of samples.
- Infographics: Infographics can present complex information in a visually appealing and easy-to-understand format. They can be used to illustrate the stages of cervical cancer, the benefits of screening, and the patient journey. The infographic could compare and contrast the Pap test and the HPV test, highlighting the advantages of each.
- Community Workshops and Seminars: These events provide an opportunity for women to learn about cervical cancer screening in a group setting and ask questions. They can be led by healthcare professionals or trained community health workers. The workshops should incorporate interactive elements, such as Q&A sessions and group discussions.
Common Misconceptions and Fears
Many women have misconceptions or fears about cervical cancer screening that can deter them from getting screened. Addressing these concerns is crucial.
- Fear of Pain: Some women fear that the Pap test will be painful. Explaining that the procedure is usually quick and may cause only mild discomfort can help alleviate this fear. The healthcare provider should reassure the patient that they will be as gentle as possible.
- Embarrassment: Many women feel embarrassed about the examination. Providing a comfortable and private setting and explaining the procedure in a sensitive manner can help reduce this feeling. The healthcare provider should maintain a professional and respectful demeanor throughout the process.
- Fear of Results: Some women worry about receiving a positive result. Explaining that a positive result doesn’t always mean cancer and that further testing is often required can help manage this fear. The healthcare provider should emphasize that early detection is key to successful treatment.
- Misunderstanding of the Process: Some women are unsure about what happens during the screening. Clear explanations and visual aids can help clarify the process. The healthcare provider should explain the difference between a Pap test and an HPV test.
- Belief that Screening is Unnecessary: Some women may believe they are not at risk or that screening is unnecessary if they feel healthy. Emphasizing that cervical cancer can develop without symptoms and that screening is the best way to detect it early is crucial. Healthcare providers should highlight that HPV is a very common virus, and even women with no symptoms can be infected.
Patient Journey Flowchart
The patient journey from screening to diagnosis and treatment can be visualized through a flowchart. This flowchart helps women understand the steps involved and what to expect at each stage.
Flowchart Description:
The flowchart begins with the “Initial Screening (Pap Test and/or HPV Test)” box.
- If the screening result is “Negative/Normal,” the flowchart proceeds to “Routine Screening as per guidelines.”
- If the screening result is “Abnormal,” the flowchart proceeds to “Further Evaluation.”
Further Evaluation:
- Colposcopy: If the further evaluation includes a colposcopy, the flowchart proceeds to “Biopsy (if needed).”
Biopsy (if needed):
- Biopsy Results:
- If the biopsy results indicate “No Cancer/Precancer,” the flowchart proceeds to “Follow-up/Surveillance.”
- If the biopsy results indicate “Precancer,” the flowchart proceeds to “Treatment.”
- If the biopsy results indicate “Cancer,” the flowchart proceeds to “Cancer Staging and Treatment Planning.”
Treatment:
- Treatment options for precancerous lesions may include loop electrosurgical excision procedure (LEEP), cryotherapy, or other procedures.
Cancer Staging and Treatment Planning:
- Cancer staging determines the extent of the cancer. Treatment options depend on the stage of the cancer and may include surgery, radiation therapy, chemotherapy, or a combination of these.
Outcomes:
- Negative/Normal result: The patient continues with routine screening as per the guidelines.
- Precancer treatment: The patient receives treatment for precancerous lesions.
- Cancer treatment: The patient receives treatment for cancer.
The flowchart should be presented in a clear, concise, and easy-to-understand format. It should include clear labels for each step and arrows to indicate the flow of the process. The flowchart can be included in educational materials, such as brochures and websites. This patient journey flowchart helps to reduce anxiety and promote informed decision-making.
Challenges and Considerations for Implementing the Age Change
Implementing the new cervical cancer screening guidelines, which lower the screening age to 25, presents both opportunities and challenges for healthcare providers and the healthcare system. Careful planning and resource allocation are essential to ensure a smooth transition and maximize the benefits of early detection while mitigating potential drawbacks.
Potential Challenges for Healthcare Providers
Healthcare providers may encounter several challenges when implementing the new screening guidelines. Addressing these challenges proactively is crucial for the successful adoption of the new recommendations.
- Increased Workload: Lowering the screening age will likely increase the number of women eligible for screening. This could lead to a higher volume of appointments for Pap tests and HPV tests, potentially straining existing clinic resources and staff capacity. Clinics might need to adjust appointment schedules, hire additional personnel, or extend operating hours to accommodate the increased demand.
- Resource Constraints: Increased screening demands can place a strain on existing resources. This includes laboratory capacity for processing samples, the availability of colposcopy services for follow-up, and the need for trained healthcare professionals to interpret results and provide counseling. Insufficient resources can lead to delays in diagnosis and treatment, impacting patient outcomes.
- Training and Education: Healthcare providers may require additional training to familiarize themselves with the updated guidelines, including new screening protocols and management strategies. This is particularly important for those who have been practicing under the previous guidelines. This includes updating protocols for follow-up testing and managing abnormal results in younger women.
- Patient Communication: Healthcare providers need to effectively communicate the rationale behind the age change to patients, addressing any concerns or misconceptions. This involves providing clear and concise information about the benefits of screening, potential risks, and the new screening schedule. Effective communication can improve patient adherence to screening recommendations.
- Insurance and Reimbursement: Changes in screening guidelines can sometimes lead to issues with insurance coverage and reimbursement. Healthcare providers need to be aware of the billing codes and ensure that screening services are appropriately covered by insurance providers. Delays or denials of reimbursement can create financial burdens for both providers and patients.
Cost-Effectiveness of Screening at Age 25
Comparing the cost-effectiveness of screening at age 25 versus the previous guidelines involves analyzing the balance between costs and health outcomes. Cost-effectiveness is usually measured using quality-adjusted life years (QALYs).
Studies examining the cost-effectiveness of screening programs consider factors such as:
- Screening Costs: This includes the cost of Pap tests, HPV tests, colposcopies, and other related procedures.
- Treatment Costs: The cost of treating precancerous lesions or cervical cancer, including surgery, radiation therapy, and chemotherapy.
- Health Outcomes: This refers to the number of lives saved, the reduction in cancer incidence, and the improvement in quality of life.
- Cost-Effectiveness Analysis (CEA): CEA involves calculating the incremental cost-effectiveness ratio (ICER), which is the additional cost per QALY gained. The ICER is compared to a threshold value, which is often based on what society is willing to pay for an additional year of life in good health.
Example: A hypothetical study might compare the cost-effectiveness of screening starting at age 25 with screening starting at age 30. The study could find that screening at age 25 results in a slightly higher initial cost due to increased screening frequency. However, the study could also find that screening at age 25 leads to a reduction in the incidence of advanced cervical cancer, resulting in lower treatment costs and improved survival rates.
If the ICER for screening at age 25 is below the accepted threshold, it would be considered cost-effective.
Ensuring Equitable Access to Screening Services
Ensuring equitable access to cervical cancer screening is paramount to reducing disparities in health outcomes. This involves addressing barriers that may prevent certain populations from accessing screening services.
- Reaching Underserved Communities: Targeted outreach programs are essential to reach women in underserved communities, such as those in rural areas, low-income populations, and minority groups. This may involve mobile screening clinics, community health workers, and culturally sensitive educational materials.
- Addressing Language Barriers: Providing information and services in multiple languages is crucial to ensure that all women can understand the benefits of screening and how to access services. This includes translating educational materials, providing interpreters, and employing healthcare professionals who speak multiple languages.
- Reducing Financial Barriers: Addressing financial barriers is critical. This involves ensuring that screening services are covered by insurance, offering financial assistance to low-income patients, and providing free or low-cost screening options.
- Addressing Transportation Challenges: Providing transportation assistance or offering screening services at convenient locations, such as community centers or workplaces, can help overcome transportation barriers. Telehealth consultations can also be utilized to increase access to care.
- Increasing Awareness and Education: Raising awareness about cervical cancer and the importance of screening is crucial. This can be achieved through public health campaigns, educational programs, and partnerships with community organizations.
Perspectives of Healthcare Providers and Patients
Understanding the perspectives of both healthcare providers and patients is essential for a successful implementation of the age change. Here’s a blockquote that provides a glimpse of these viewpoints:
“As a healthcare provider, I welcome the change to screening at age 25. Early detection is crucial, and this will help us catch potential problems sooner. However, I am concerned about the increased workload and the need for more resources. We need to ensure that we have the staff and infrastructure to handle the increased demand.”
– Dr. Emily Carter, Gynecologist“I understand the need for earlier screening, but I was a bit confused when I first heard about the change. I am concerned about unnecessary tests and the potential for anxiety. I want to make sure I understand the process and what the results mean.”
– Sarah Miller, Patient“I’m a bit nervous about starting screening at 25, but I understand that it’s important. I want to be healthy and prevent any serious problems down the road. I hope that the new guidelines are effective and that I can easily access the services.”
– Maria Rodriguez, Patient
Comparison with International Screening Guidelines
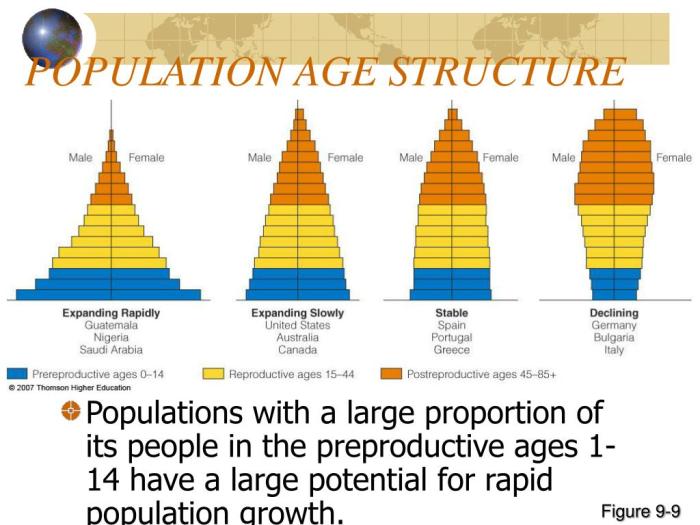
Source: slideserve.com
Lowering the cervical cancer screening age to 25 in some regions necessitates a broader understanding of international best practices. Comparing guidelines across different countries reveals variations in screening age, methods, and frequency, each impacting cervical cancer incidence and mortality. Examining these differences offers valuable insights for optimizing screening programs.
Similarities and Differences in Screening Guidelines
The approach to cervical cancer screening varies considerably across nations. While the goal of early detection is universal, the specific strategies employed reflect diverse healthcare systems, resources, and epidemiological profiles.
- United States: The US Preventive Services Task Force (USPSTF) recommends starting screening at age 25 with primary HPV testing every 5 years, co-testing (HPV and Pap) every 5 years, or Pap tests every 3 years. This shift towards primary HPV testing reflects the higher sensitivity of this method.
- United Kingdom: The UK’s National Health Service (NHS) offers cervical screening to women aged 25 to 64. Screening is primarily based on cytology (Pap smears) every 3 years for those aged 25-49 and every 5 years for those aged 50-64.
- Canada: Screening guidelines vary slightly across provinces and territories. Generally, screening begins at age 25 or when a woman becomes sexually active. The preferred method is HPV testing, with a frequency of every 3-5 years, depending on the province and test results.
- Australia: Australia implemented a significant change in 2017, moving to primary HPV testing every 5 years for women aged 25-74. This replaced the previous Pap smear-based screening program.
Impact of Screening Guidelines on Cancer Incidence and Mortality
Differences in screening guidelines demonstrably influence cervical cancer incidence and mortality rates. Countries with more comprehensive and frequent screening programs, especially those utilizing HPV testing, often experience lower rates of both.
- Australia’s Success: The shift to HPV testing in Australia has been associated with a significant decrease in cervical cancer incidence. Early data suggests a reduction in the number of cases due to the higher sensitivity of HPV testing.
- UK’s Progress: The UK has seen a steady decline in cervical cancer mortality over several decades, largely attributed to its well-established screening program. However, variations in uptake and access can still lead to disparities.
- US Variability: The US, with its diverse screening approaches and varying access to healthcare, experiences variations in outcomes. Regions with higher screening rates tend to have lower cervical cancer incidence.
Innovative International Screening Approaches
International initiatives highlight innovative screening methods that could be adapted.
- Self-Sampling: Several countries, including the UK and Australia, are increasingly using self-sampling for HPV testing. This involves women collecting their own samples at home, improving access and uptake, particularly in underserved populations.
- Primary HPV Testing: The widespread adoption of primary HPV testing, as seen in Australia and the US, has proven effective in identifying women at risk. This method is more sensitive than cytology alone, leading to earlier detection.
- Artificial Intelligence (AI): Some countries are exploring the use of AI to analyze Pap smear slides, potentially improving the accuracy and efficiency of screening.
Comparison Table of Screening Guidelines
Below is a comparative table of cervical cancer screening guidelines across several countries.
| Country | Age Range | Screening Method | Frequency |
|---|---|---|---|
| United States | 25+ | Primary HPV test, Co-testing (HPV and Pap), Pap test | Every 5 years (HPV), Every 5 years (co-testing), Every 3 years (Pap) |
| United Kingdom | 25-64 | Cytology (Pap smear) | Every 3 years (25-49), Every 5 years (50-64) |
| Canada | 25+ (or when sexually active) | HPV testing | Every 3-5 years (depending on province/test results) |
| Australia | 25-74 | Primary HPV testing | Every 5 years |
Final Wrap-Up
In conclusion, the decision to lower the cervical cancer screening age to 25 represents a proactive step towards enhancing early detection and improving women’s health. By understanding the reasons for this change, the screening process, and the importance of patient education, we can work together to increase awareness and ensure equitable access to this potentially life-saving screening. This proactive measure promises a future with fewer cervical cancer diagnoses and improved outcomes for women.
FAQ Summary
Why was the screening age lowered to 25?
The age was lowered based on updated medical research showing that screening at 25 can detect early signs of cervical cancer in younger women, leading to better outcomes.
What screening methods are used at age 25?
The primary methods are Pap tests and HPV tests. Your doctor will discuss the best option for you.
How often should I get screened if I’m 25 or older?
The frequency depends on the specific screening method and your individual risk factors. Your doctor will advise you on the appropriate schedule.
What happens if my screening results are abnormal?
Abnormal results require follow-up, which might include additional tests or procedures. Your doctor will explain the next steps based on your results.
Is screening at 25 covered by insurance?
Most insurance plans cover cervical cancer screening. It’s always a good idea to check with your insurance provider to confirm coverage.